POLST Paradigm Initiative Reaches from Oregon to NC
June 22, 2006
 As
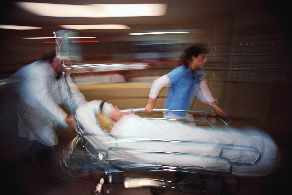
we reported in March, Oregon's end-of-life orders document
— "POLST"— is being proposed in a number
of states across the US. In North Carolina, the form
has undergone pilot tests, and the North Carolina Medical
Society is considering its adoption. As
we reported in March, Oregon's end-of-life orders document
— "POLST"— is being proposed in a number
of states across the US. In North Carolina, the form
has undergone pilot tests, and the North Carolina Medical
Society is considering its adoption.
The purpose of this letter is to
- Review the history of POLST on a national level
- Update you on the status of North Carolina's version
of POLST
POLST: the ultimate pink slip
 POLST
is an end-of-life orders document. It is a form —
along with a coaching process — to convert advance
directives into physician's orders as a patient's condition
changes. POLST was devised in Oregon in the 1990s under
grants from the Greenwall Foundation and Cummings Foundation,[1]
frequent sponsors of right-to-die organizations. POLST
is an end-of-life orders document. It is a form —
along with a coaching process — to convert advance
directives into physician's orders as a patient's condition
changes. POLST was devised in Oregon in the 1990s under
grants from the Greenwall Foundation and Cummings Foundation,[1]
frequent sponsors of right-to-die organizations.
The POLST Task Force emphasizes that the POLST form
is not an advance directive, which means that in Oregon
— and many other states — it is not bound
by state advance directive statutes which often require
the patient's signature.[2]
Assisted-suicide proponent Ann Jackson testified before
a Senate subcommittee this past May on the success of
the Oregon Death with Dignity Act. In the course of
her testimony, she said that one of Oregon's successes
was POLST. According to Jackson, "respect for end-of-life
wishes is virtually 100% when POLST...is in place."
[3]
No wonder there is 100% compliance with POLST.
POLST forms are typically written as the patient's condition
changes; frequently they are written when the patient
and/or his agent are under duress. So, for example,
as a patient is going into a crisis, an EMT or nurse
or respiratory therapist might counsel the patient —
or surrogate — on next steps with regard to accepting
a feeding tube or respirator. POLST instantly converts
these "wishes" into physician's orders. Naturally,
the orders are usually followed. However, one wonders
whether the same "wishes" would have been expressed
by a more informed patient, counseled in less stressful
circumstances.
According to the POLST website (www.polst.org), some form of POLST has been endorsed by the
following states or regions: Oregon, Washington state,
West Virginia, sections of NY, Wisconsin, and Pennsylvania.
The following states are developing programs: NH, MI,
HI, NV, UT, NE, MO, TN, NC, GA, and FL. The forms may
be implemented voluntarily through medical boards, and/or
via direct legislation.
North Carolina's End-of-Life Orders document "MOST"
 When
we last wrote to you, the North Carolina end-of-life
document was named POST (Physician's Orders for Scope
of Treatment). The document has been reviewed, amended,
and approved by the North Carolina Medical Society's
Ethical and Judicial Affairs Committee. The document
is scheduled to be returned to the Task Force, and there
may be other reviews and changes in its future before
implementation. When
we last wrote to you, the North Carolina end-of-life
document was named POST (Physician's Orders for Scope
of Treatment). The document has been reviewed, amended,
and approved by the North Carolina Medical Society's
Ethical and Judicial Affairs Committee. The document
is scheduled to be returned to the Task Force, and there
may be other reviews and changes in its future before
implementation.
We have attached the newest
version of the North Carolina document to this newsletter.
The document's name, which was POST in March, has changed
to "MOST" (Medical Orders for Scope of Treatment).
There are also a few other changes in addition to the
name change. Next week we will post a full discussion
of MOST on our website (www.lifetree.com). In the
meantime, here are changes we've noted:
- The name has changed from POST to MOST (change from
"Physician's orders" to "Medical Orders")
- Signature was "optional;" signature is now "preferred."
However, the form is "still effective without signature,"
and at that, the signature can be that of a "Person,
Parent of Minor, Guardian, Health Care Agent, Spouse,
or Other Personal Representative."
- Informed consent: Statement to be signed by
patient/proxy now begins "I agree that adequate information
has been provided..." and ends with "This document
. . . indicates informed consent." (Q: Is the
patient really as well informed as the boilerplate
statement indicates?)
- Where the POST form referred to "physician", the
MOST form expands to "physician (MD/DO), physician
assistant, or nurse practitioner."
Bottom line, these forms are being tested across North
Carolina. LifeTree does not endorse the POLST
program at all, and does not recommend the adoption
of the MOST form. If it is really true that too many
patients are being forced into life-saving technologies
at the end of life, this form does not solve the problem.
The form will often be completed under duress, without
full information, and further corrodes communication
between the primary physician and his or her patient.
Pro-life physicians should be made aware of what the
NC Medical Society is trying to move into the system.
God bless you.
Betty and Ione
Elizabeth D. Wickham, PhD, Executive Director
Ione Whitlock, Chief Research Associate
LifeTree, Inc.
____________
Endnotes:
[1] "History of POLST Paradigm Project" at POLST Paradigm website,
maintained by the Center for Ethics in Health Care at
the Oregon Health & Science University; also Recent Developments in Physician-Assisted Suicide, June,
1998, "Medical Developments," #10 at Willamette University's
web site.
[2] See "Information for Health Care Professionals" at the POLST Paradigm
website; also, S. Tolle, S. Hickman, J. Newman,
The National POLST Paradigm Initiatve, page 4. For
a history of POLST in Oregon, and what to look for in
other states, see State
Initiatives in End-of-Life Care, Issue 3, April
1999, "Implementing End-of-Life Treatment Preferences
Across Clinical Settings."
[3] Testimony of Ann Jackson, MBA, Executive Director, Oregon
Hospice Association, before the Senate Committee on
Judiciary Subcommittee on the Constitution, Civil Rights,
and Property Rights, “The Consequences of Legalized
Assisted Suicide and Euthanasia”, Thursday, May
25, 2006.
"When inevitable death is imminent
in spite of the means used, it is permitted in conscience
to take the decision to refuse forms of treatment that
would only secure a precarious and burdensome prolongation
of life as long as the normal care due to the sick person
in similar cases is not interrupted. "Declaration on Euthanasia,
May 5, 1980
"The evaluation of probabilities, founded on waning hopes
for recovery when the vegetative state is prolonged beyond
a year, cannot ethically justify the cessation of interruption
of minimal care for the patient, including nutrition and
hydration. Death by starvation or dehydration is, in fact,
the only possible outcome as a result of their withdrawal.
In this sense it ends up becoming, if done knowingly and
willingly, true and proper euthanasia by omission, "Address
of John Paul II to the Participants in the International
Congress on "Life-Sustaining Treatments and Vegetative
State: Scientific Advances and Ethical Dilemmas," Saturday,20,
March 2004
|
 |







